Restructuring Healthcare Delivery with Mobility and AR
A recent Lancet study reveals that five billion people across the world continue to have no access to safe and affordable surgery. Another report highlights only 2.2 million surgeons, aestheticians, and obstetricians perform 143 million simple operations annually—a significant infrastructural burden. The situation only worsens at the rural level across developing economies. A study published by Journal of Perinatology paints an alarming picture of the state of newborn health and access to maternal healthcare in India. With about 0.75 million neonates dying every year—a record high for any country—the rural population remains consistently disadvantaged. Insufficient man power at heath facilities, inadequate funding, and poor governance continue to hinder equitable access to affordable or free healthcare. Due to these ground realities, the healthcare sector is experimenting with telemedicine delivery models that can close the glaring gap between patient demand and provider supply. In fact, the first documented case of telesurgery can be traced back to 2001. Dr. Jacques Marescaux performed a gall bladder surgery from New York on a patient located in a hospital in France. There were, however, several drawbacks—the biggest being the communication lag time. Existing telecommunication networks make it difficult to keep the time latency below the required 105 milliseconds to avoid deterioration in performance and patient experience.
Creating Dialogue: Connecting Patients and Providers
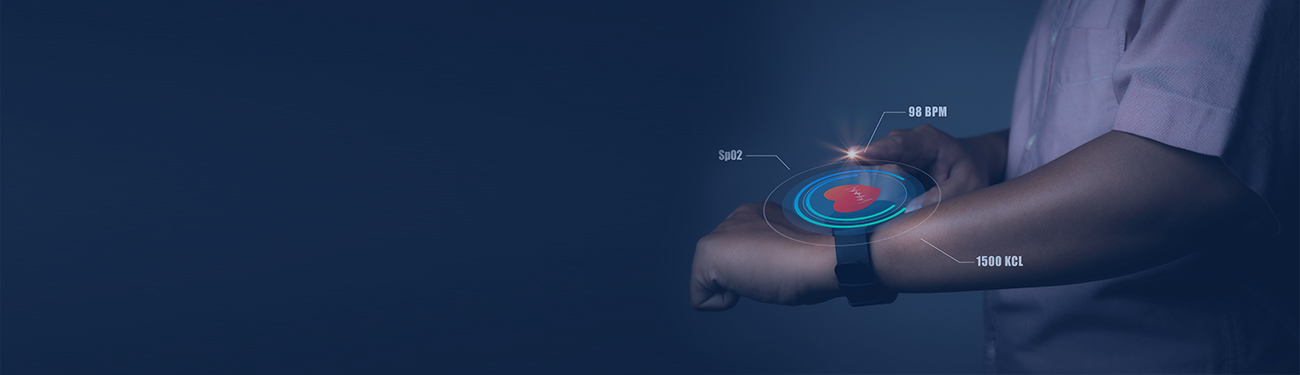
With 5G networks promising to bring down latency to a few milliseconds, it is now possible to remotely consult, diagnose, treat, and intervene with greater accuracy and reliability. This lays the foundation for implementing mobility and augmented reality (AR) solutions on an unprecedented scale. Da Vinci robots represent the perfect convergence of these two solutions, enabling professionals to perform remote surgeries in medically-isolated locations, war zones, and even space. Researching the benefits of telemedicine for managing chronic conditions, the Veterans Administration (VA) observed a number of other positive outcomes. The telehealth program helped reduce bed stay by 25%, minimize hospital admissions by 19%, and enhance patient satisfaction scores by 86%. To further strengthen the argument, a research study by the University of California quantified the benefits of this concept in terms of cost, not just outcome. It found that ICU telemedicine yielded cost savings in 37% of the 1000 test scenarios. To test the reach of telemedicine, Warmington et al published a report detailing the feasibility of an arthritis education program. This study was conducted on aging patients suffering from inflammatory arthritis, residing in remote areas with limited connectivity. The interview data collected from participants demonstrated the social and educational benefits, and highlighted that such care would have been inaccessible without telemedicine. Creating a holistic, patient-centric care model hinges not just on delivery but the ability to remotely, and non-intrusively capture and transmit critical patient data. With one out of every six consumers using wearable technology, leveraging the connected devices ecosystem is an obvious starting point. These devices are designed to remotely monitor bio signals without user intervention. Advances in sensor technology and microelectronics can also increase the fluency of dialogue between consumers and healthcare providers. Following a similar approach, other players in the healthcare value chain such as pharmaceuticals could eventually be brought into the fold. Take the case of Tech Tats that combines the pure aesthetics of traditional tattoos with the functionality of wearables. These are not only easier to wear, but their electro-conducive paint contains a variety of sensors that help monitor the user’s vital stats. If providers chose to share this information over a closed network, patient data becomes accessible, minimizing instances of error, effort duplication, and in the long run, readmission. However, to completely harness the full potential of telemedicine, healthcare providers will need to complement it with AR.
Re-imagining Realities: ‘Seeing Through’ the Patient
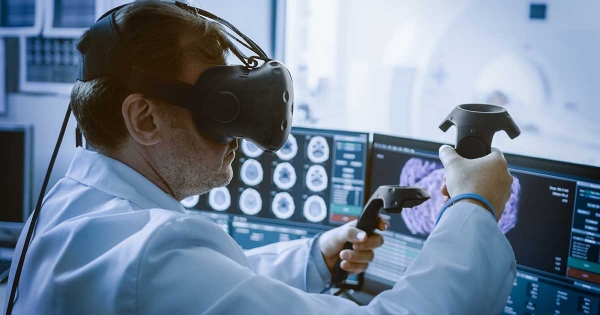
AR promises to grant unparalleled insights into the human anatomy. The technology is already in use by certain start-ups to develop non-intrusive vein scanners, which can improve first-time vein hit success rate by 3.5 times. Last year, Dr. Shafi Ahmed, a surgeon at The Royal London Hospital excised a tumor from the liver and bowel of a patient in the world’s first operation streamed online using a pair of AR glasses. The glasses allowed him to broadcast this live for roughly 14,000 students in 32 countries, giving them an opportunity to interact and directly raise questions to him as he performed the operation. Theoretically, the uses of AR can be extended to pharmas and other complementary segments of the medical industry. Dispensaries can use camera-based mobile applications for scanning and recording prescriptions, and for quickly accessing drug and inventory information. Lab workers remotely controlling and monitoring experiments as well as drawing test results can minimize risks while handling hazardous materials. In addition, self-diagnosis can be improved by equipping patients with AR-enabled wearables to monitor various parameters. In context of the consumer market, the growing aged population presents a number of opportunities for implementing AR. Utilizing wearables and apps, AR can take the patient self-care process to the next level. Encouraging physical activities, providing reminders for everyday tasks, and even organizing dosage schedules are just some of the possibilities.
Reapplying the Connections: Monitor, Sustain, Service
Within the medical industry itself, the same integrated sensors, which are used to record patient data can be leveraged to record device data. Remote machine health monitoring can be applied by engineering and servicing teams to execute sustenance and upkeep activities—utilizing data-driven forecasts to perform predictive maintenance and optimize equipment uptime. Adopting a proactive maintenance approach, companies can ensure that field support staff place replacement orders for damaged components in near real-time, without stepping out of their stations. They can also use AR-enabled headsets to scan faulty machine and run failure mode simulations for root cause analysis, significantly diminishing pressure on their bottom lines. Evidently, the confluence of mobility and AR has applications that not only address healthcare challenges, but grant complete visibility into patient and business health.